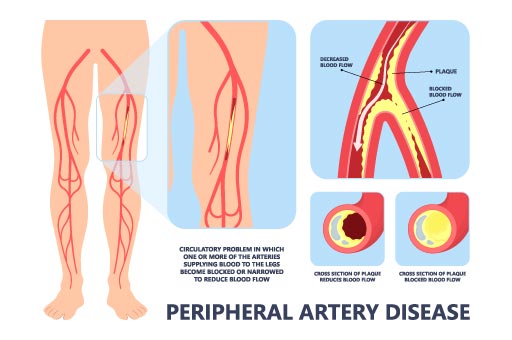
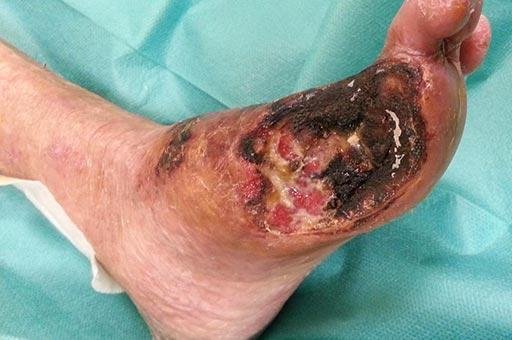
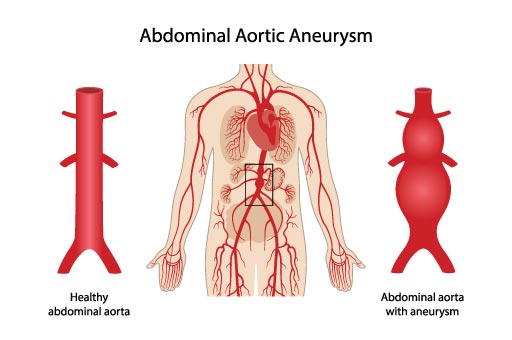
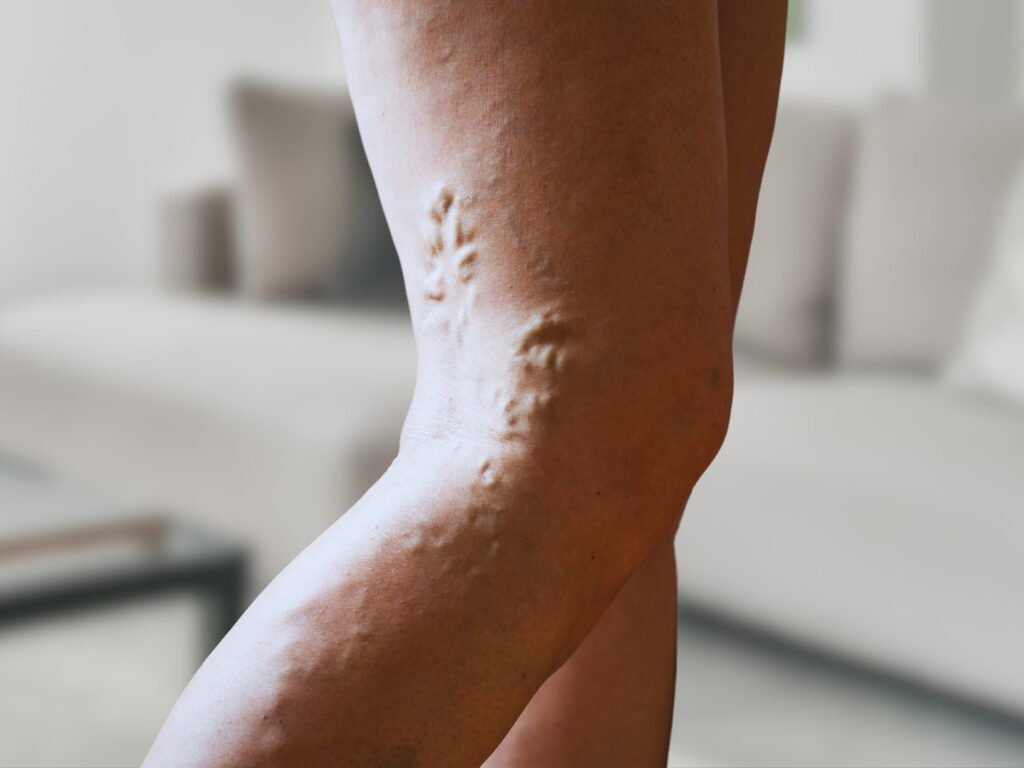
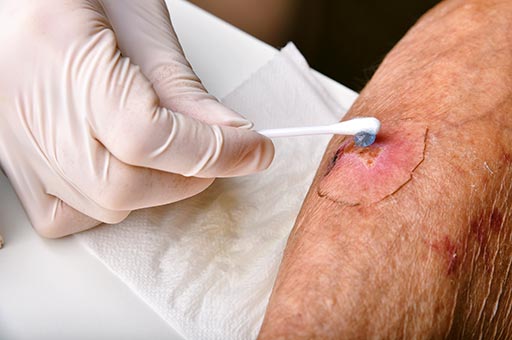
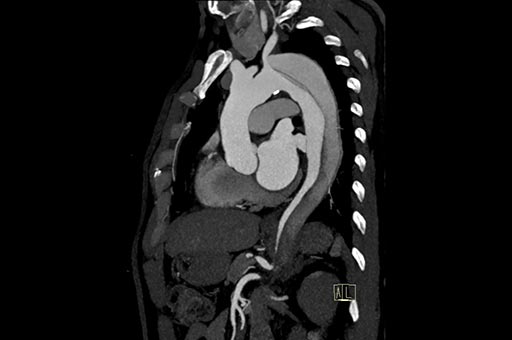
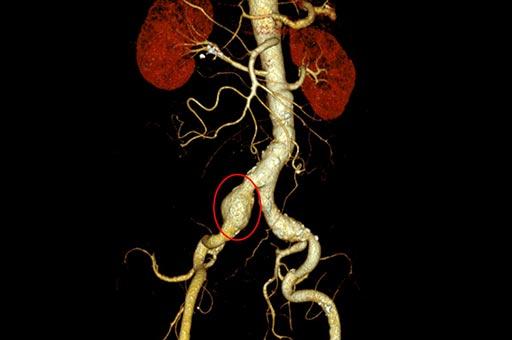
These conditions primarily affect the arteries, which are blood vessels responsible for transporting oxygenated blood from the heart to the rest of the body. The aorta, the body’s main and largest artery, can be afflicted by various conditions that compromise its function and structural integrity. These conditions can manifest in various ways, from minor symptoms to life-threatening events. Early diagnosis and treatment are crucial to prevent life-threatening complications.